Outreach efforts done by CBC News on global academics who have studied in and teach courses on Canada reveal that Canada is globally praised for its universal, inclusive healthcare. Yet the recently announced Canadian federal budget for 2017 continues to grapple with health issues plaguing Canadian stakeholders, and some needs are addressed better than others. Indigenous peoples and health researchers are two groups particularly affected by the healthcare allocations in the new budget.
In this year’s budget, a substantial amount of capital was dedicated to improving healthcare for Indigenous populations: close to $830 million over the next five years has been committed towards expanding healthcare resources for First Nations and Inuit communities. This includes investing in repair and improvement of healthcare infrastructure, while incorporating other services for mental health, addiction, and culturally-appropriate health services.
Budget 2017 seems to hit most of the important points facing Indigenous health today – especially those living on reserves and in remote communities. Teen suicide on and off reserves has brought attention to the alarming rate of mental health issues Indigenous communities are faced with. Across Canada, Indigenous suicide rates are six to eleven times that of the rest of Canada. Depression is also found at double that of the Canadian average. With Budget 2017 allocating close to $120 million toward mental health plus another $205 million to culturally specific healing (together 39% of the $830 million), hopefully significant strides can be made to mitigate mental health issues in Indigenous communities.
The $205 million for culturally specific healing will go towards non-insured medical care – including for the first time ever, traditional Indigenous healers. Traditional healing presents a holistic model of wellness, integrating the mind, body and environment in community-specific ways. For instance, a focus on diet, oral history and the use of plant-based medicines would fall under this model.
Traditional healing remains important for its emphasis on holistic care, which is helpful for treating mental health issues. In remote communities with limited access to hospitals or clinics, traditional healers are also important for their community-specific familiarity. Furthermore, the budget’s $15 million allocation towards addiction and harm reduction services will provide adequate expenditure to deal with high rates of substance abuse in several Indigenous communities as well.
Where Budget 2017 falls short is in reforming existing health structures to be more inclusive for indigenous members as well. There appear to be significant systemic factors which plague the way Indigenous people are treated in the healthcare system. Maltreatment of Indigenous people going through the healthcare system has been brought to light in recent years by inquiries and inquests into indigenous deaths. In one particular case, an indigenous man named Brian Sinclair, who suffered for 34 hours in an emergency room for a treatable bladder infection, was left unexamined until he was pronounced dead. The man’s family is certain racism is the cause for the ill treatment of Brian and call for a deeper look into its effect on healthcare institutions in Canada.
A recent book by University of Toronto professor Dr. Sherene Razack argues that the legacy of settler-colonialism still plagues the way Indigenous peoples are treated in western institutions. Furthermore, for many remote Indigenous communities, the geographical barriers of access to healthcare institutions has a large impact on the quality of care they are able to receive.
Culturally sensitive and appropriate solutions are necessary, and while a portion of the $830 million for Indigenous healthcare goes towards culturally appropriate healthcare initiatives, the services that emerge will have to work together with the institutional healthcare system to assure Indigenous members are treated fairly.
A sizeable segment of the healthcare budget is allocated towards Indigenous healthcare – and if utilized well it can lead to great leaps in Indigenous people’s health. Health researchers on the other hand may be disappointed with allocations in the 2017 budget. In total, $544 million is dedicated towards prescription medications and health innovation, although most of that goes towards offsetting prescription costs and making healthcare and prescription services more digital. Over the next three years, only $51 million will be allocated towards accelerating health innovation throughout the country. This is coupled with close to $14 million over four years dedicated towards innovation for veterans. Specifically, a Veteran and Family Well-Being Fund will be established to support the research and development of innovative programs to support veterans and their caregivers, both mentally and physically.
Compared to the US, UK and Australia, Canada has dedicated the lowest proportion of their total health expenditure towards health research. With only 2.9% of total health expenditure going towards health innovation, as opposed to 4.5% in the US, for instance, Canada has deemed innovation in healthcare as one of the lowest priorities. While Canada is globally recognized and praised for its universal and inclusive healthcare system, the level and speed of global innovation makes it necessary for Canada to invest more capital into healthcare innovation or risk being left behind.
Healthcare innovation and technology has the long-term potential to do more with fewer resources: to reduce costs of healthcare while concurrently improving the quality of life of all Canadians. Budget 2017 has allocated a substantial amount of capital into digitizing healthcare and prescription services. While this will lead to a more efficient system, it is not the type of innovation which will solve some of the most pressing health problems Canadians are currently faced with. With the baby boomer generation aging, Canada now has more citizens over the age of 65 than under 15. New, innovative solutions are the only way to assure all seniors are living the best quality of life, later into life.
A larger investment of capital into healthcare innovation and research will also support Budget 2017’s objective of getting more youth – especially women – into Science, Technology, Engineering and Math (STEM) fields, as it pushes and supports the tangible impact of STEM education. If Canada wishes to remain a strong frontrunner for universal healthcare, it is necessary to invest in healthcare innovation, particularly research and development on a national level, or run the risk of Canadian healthcare no longer being sustainable.
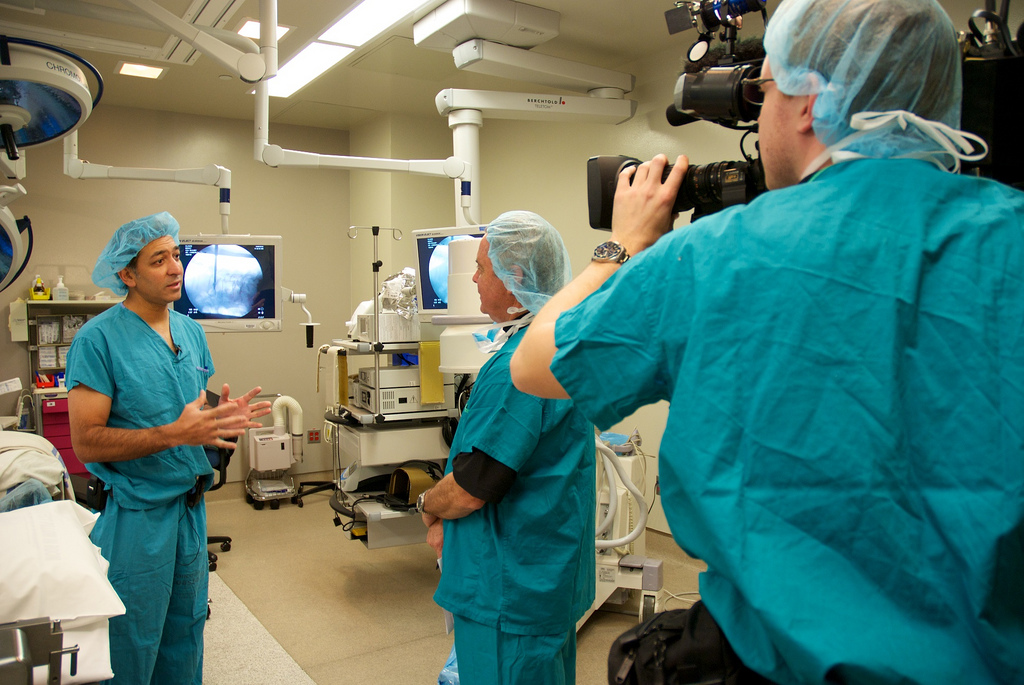
Photo: Lions Gate Hospital (April 6, 2010) by Vancouver Coastal Health via Flickr. Licensed under CC BY-NC-ND 2.0.
Disclaimer: Any views or opinions expressed in articles are solely those of the authors and do not necessarily represent the views of the NATO Association of Canada.