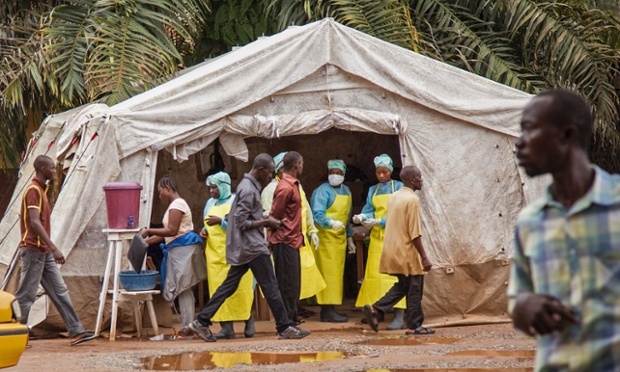
This month, the World Health Organization (WHO) breathed a small sigh of relief as news broke that the Ebola epidemic has subsided. The WHO declared Liberia Ebola-free after 42 consecutive days of no new cases of the illness, and Sierra Leone and Guinea reported fewer than 10 cases a week, the lowest levels since September 2014. Although an end to the Ebola crisis is in sight, the work is far from over. As the international community works to further reduce Ebola cases, there is a golden opportunity to ensure that future epidemics do not reach the same level of devastation.
The outbreak of Ebola began in December 2013, killing an estimated 11,000 people in West Africa and creating roughly 15,600 survivors who are dealing with its aftermath. The WHO’s emergency medical response to the epidemic was the largest of its kind, costing nearly $1 billion and requiring an unprecedented number of health care workers and volunteers.
Unfortunately, however, this response came far too late, even after repeated public warnings from Médecins Sans Frontières (MSF). The WHO waited more than three months after MSF called for the Ebola outbreak to be declared a public health emergency of international concern. Even at this point, when the death toll was rising at an unprecedented rate, the WHO concentrated on logistics, analysis, and social mobilization rather than pulling together resources to treat the illness.
In addition to being sluggish, the WHO’s response failed to prioritize the mobilization of those resources that would have been most effective in containing the virus. At the most critical point of the outbreak, MSF repeatedly stated that doctors and nurses were needed more than money. Yet medical volunteers from across the world were difficult to come by, partly because of the fear, stigma, and policy obstacles that dissuaded health care professionals from participating. The countries hardest hit by the virus often struggled with minimal or non-existent protective gear and medical equipment, as well as a lack of capable nurses and doctors to provide treatment.
 The WHO’s flawed response to the Ebola outbreak resulted in criticism from several experts, who argued that a more prompt and pragmatic action plan could have significantly reduced the death toll. In response, the WHO has taken steps to improve its ability to address future major crises, most of which have involved reversing funding cuts to better support emergency response departments and establishing a contingency fund so that financial resources will be available in the event of another outbreak. The organization also seeks to create a new program that will mandate performance expectations for what will be required to happen 24, 48, and 72 hours after an outbreak is declared.
The WHO’s flawed response to the Ebola outbreak resulted in criticism from several experts, who argued that a more prompt and pragmatic action plan could have significantly reduced the death toll. In response, the WHO has taken steps to improve its ability to address future major crises, most of which have involved reversing funding cuts to better support emergency response departments and establishing a contingency fund so that financial resources will be available in the event of another outbreak. The organization also seeks to create a new program that will mandate performance expectations for what will be required to happen 24, 48, and 72 hours after an outbreak is declared.
In search of further improvements, German Chancellor Angela Merkel has recently established a panel of world experts to formulate a plan for reform. New changes involve the creation of a new, semi-autonomous body within the WHO that will take over the responsibility of warning the world of future disease epidemics. This new body, which will have a high degree of independence and operate with its own funding and directorship, will decide whether a disease outbreak requires the attention of the international community. To make this task easier, the body will also seek to ensure all countries have proper disease surveillance systems, and will be in charge of deploying carefully planned global health workforces in the event of another epidemic.
Shifting this responsibility to an independent body should allow for a more focused and effective response to global health crises. It may also give individual countries an enhanced ability to carry out their own preliminary emergency responses and analyses before additional support and resources arrive on the ground.
In analyzing the handling of the Ebola epidemic, it is clear that the WHO was ill-equipped to deal with the very sort of medical catastrophes it was established to prevent. After a thorough investigation, a United Nations-commissioned panel of experts was still unable to determine why the WHO was unresponsive to early warnings during the crescendo of the outbreak in early 2014. Nevertheless, these preliminary reform measures show that the Ebola epidemic served as a watershed moment for the WHO and other international organizations. With the benefit of hindsight, a coordinated and streamlined process will hopefully contain future epidemics.